Also known as key-hole gallbladder removal
Laparoscopic cholecystectomy (key-hole gallbladder removal) is an advanced key-hole surgery that is currently performed by the surgeons at Anderson Moores. The procedure is performed via a small 2.5-3cm incision just behind the umbilicus (this slightly bigger incision size is needed to allow extracting the diseased gallbladder from the abdomen) and additional one or two very small 5-10mm incision on either side of the abdomen.
The most common indication is treatment of early gallbladder mucocele (please see the information sheet on our website for a more in-depth discussion on gallbladder mucocele). Patients with recurrent gallbladder infections (bacterial cholecystitis) are potential candidates for keyhole surgery as well.
Patients with early mucocele were historically treated medically due to concerns that open surgery is invasive and associated with a potential for serious complications. However, a conservative approach is not without risk because gallbladder mucocele tends to progress and can lead to gallbladder rupture and subsequent life-threatening peritonitis. For this reason, active monitoring with frequent abdominal scans is often necessary. The availability of keyhole surgery for gallbladder removal provides a safe option with a reduced risk of complications such as pancreatitis and allows a more rapid recovery.
Case selection is paramount and not all patients with gallbladder mucocoele are candidates for keyhole surgery. Emergency cases, cases with concern about impending gallbladder rupture and wall compromise as well as patients with significant increase of bilirubin and biliary duct distension/obstruction (who may need duct flushing via open surgery) are not suitable. Good candidates for laparoscopic cholecystectomy are cases that are elective, have early gallbladder mucocoele, no elevation or only mild elevation of bilirubin or cases with refractory bacterial cholecystitis.
Benefits are less pain, shorted hospital stay, very low to negligible risk of pancreatitis (one of the major benefits). The risk of biliary leakage and peritonitis is low but remains similar to open surgery. About 1 patient in 5 may need conversion to open surgery, mainly if it is discovered doing the keyhole procedure that the gallbladder disease is more advanced than anticipated on ultrasound.
Patients that may require key-hole gallbladder removal are generally assessed via our Internal Medicine Service first. They are transferred to the Soft Tissue Surgery Department if the indication for the procedure is confirmed after the initial investigations.
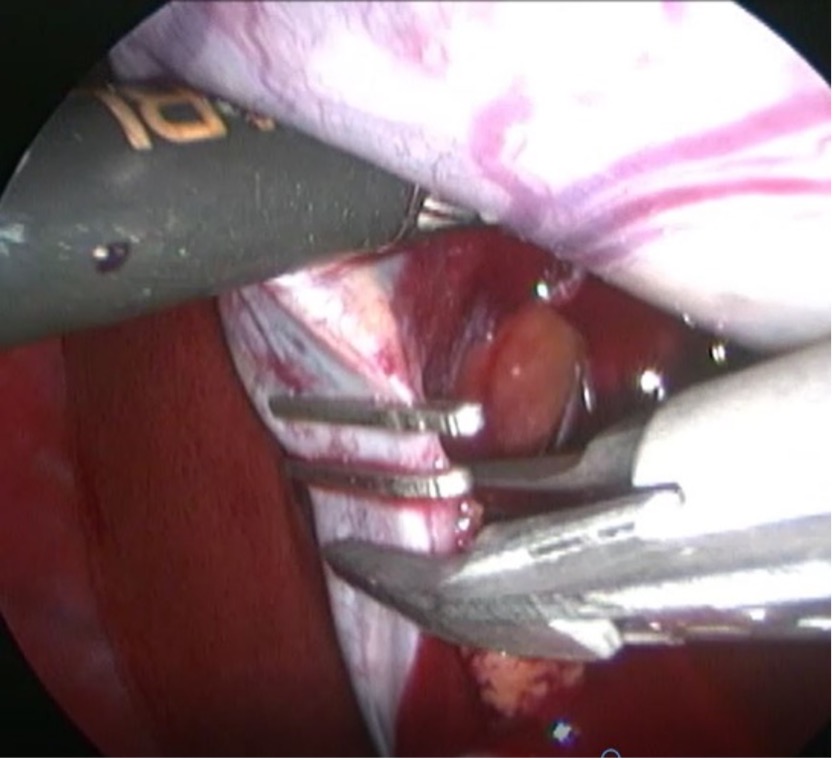
Fig 1. Laparoscopic cholecystectomy: the diseased gallbladder is retracted ventrally and a laparoscopic clip applier is used to occlude the dissected cystic duct with titanium clips in preparation for transection and gallbladder removal.
